Hone your POCUS interpretation and clinical reasoning by working through the interactive case below.
Case #18: Respiratory Failure and Volume Overload Post-Renal Transplant - It’s a Trap!
A male in his 70s with a history of ESRD on HD secondary to T2DM was admitted to hospital electively for a deceased donor renal transplant 1 month prior to the POCUS team consult. His dry weight was listed at 63.5kg. At the time of admission, vital signs and physical exam were unremarkable. His past medical history was notable for concern about ischemic heart disease, though he had no previous established MI or HF.
MIBI Aug 2023: small perfusion defect basal posterior wall
Stress echo Aug 2024: no inducible ischemia but ST elevations in inf and lateral walls. EF 60%, mod diastolic dysfxn, sev dilated LA, mod AS AVA 0.7cm, PASP 32, normal RV.
He underwent OR the next day; notes suggest this was uneventful. Post-operatively he required pressors for several hours. Creatinine decreased from 921 to 880. Hemoglobin dropped from 101 to 77. He was 4.7L fluid positive. Urine output was 600mL.
Over next couple days developed cardio-resp symptoms. Troponin rose from 1109 to 45,000 and ECG showed dynamic ST and T wave changes. He developed worsening renal function and acidosis and ended up going back on iHD POD2.
He was reviewed by Cardiology and initially felt to have a type 2 MI, but subsequently felt to be more in keeping with type 1 MI. Unfortunately he was not a candidate for intervention at that time and the recommendation was made to manage medically.
POCUS examination was recorded at that time: IVC <2cm, B lines present, mild LV systolic dysfunction. He ended up in the CCU for monitoring on POD4
In CCU his respiratory status continued to fluctuate. He was on and off BPAP and was on high-dose lasix in addition to iHD.
It is difficult to tease out from the notes, but it seems that his respiratory failure was blamed on pulmonary edema (sometimes described as flash pulmonary edema), possible pneumonia (GPCs grew in sputum - treated with amox/clav). At one point however volume overload was questioned by Nephrology as the patient continued to have episodic deterioration despite effective UF.
Eventually he stabilized and got off iHD, then moved back to the ward after 5 days in CCU.
On the ward he continued to have fluctuations in his respiratory status and his creatinine continued to rise. He was placed back on iHD a few days later. A renal biopsy was done showing acute tubular injury.
Skipping ahead a couple weeks … 1 day prior to POCUS consult the patient was now off iHD again. He remained on high dose IV lasix and metolazone. He was also being treated with pip-tazo for cough, sputum, and heavy growth of E.coli on sputum culture. Creatinine had been increasing again into the 300s. A recent echo had been done showing a dilated LV, LVEF 40% - global hypokinesis, normal RV, severe biatrial enlargement, PASP 41, E/e’ 17.3.
The POCUS team was consulted (now about 1 month into his admission) for assessment of his volume status. Current clinical data:
Rising Cr (300s), persistent SOB
Had been on Lasix 120mg IV BID and metolazone 10 for > 1 week
U/O 2,400 in past 24hrs
Afeb, breathing comfortably on 0-1L O2, RR 16, BP 133/47
+++ coughing, frequent coughing and suctioning out yellowish (?purulent) sputum
+++ LE edema to above the knees
Wt between 60 – 62Kg
His biggest complaints at the time was the cough, endorsed orthopnea
CXR the day of the consult:
Radiology report:
Initial POCUS EXAM
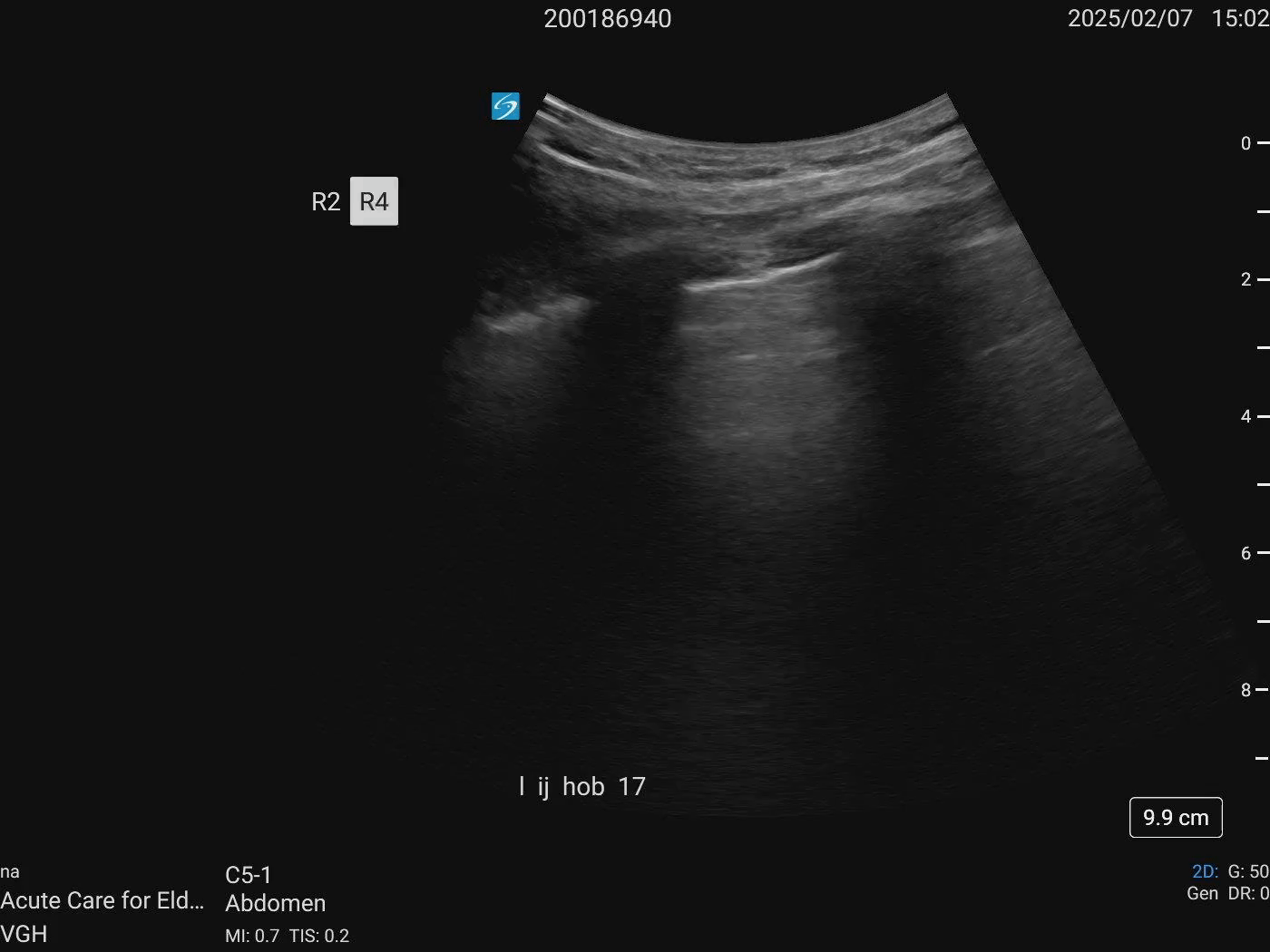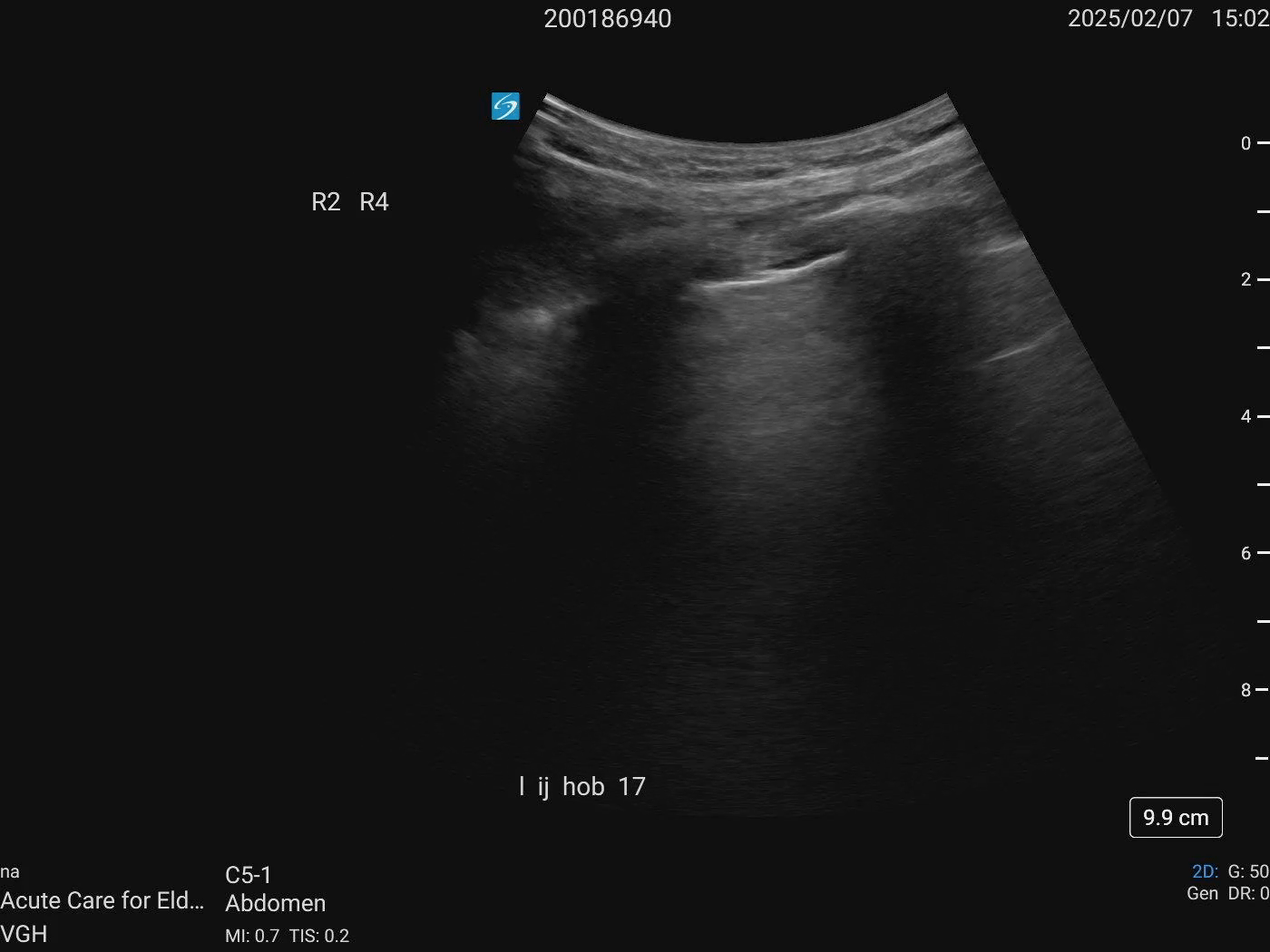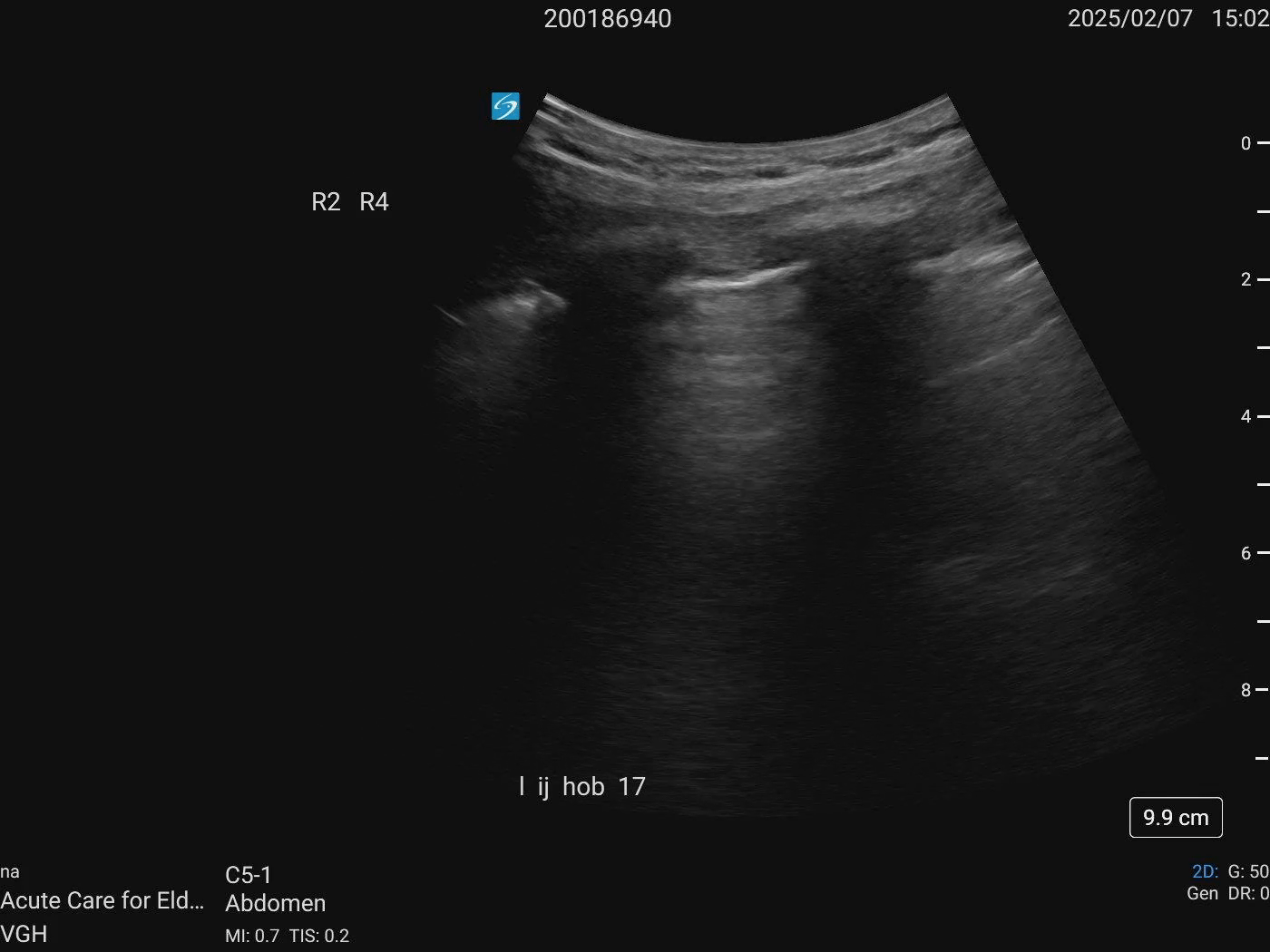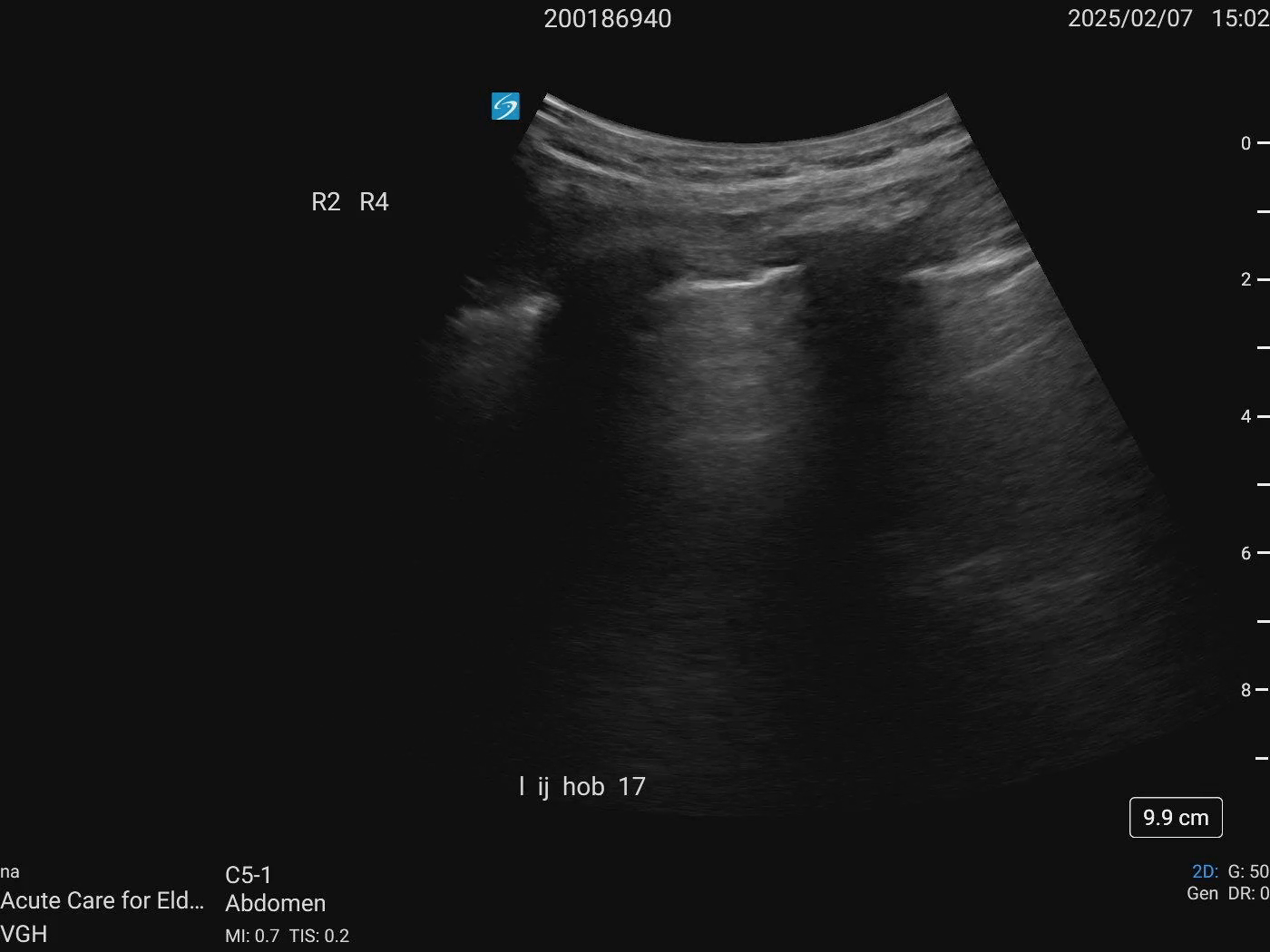
IJ: HOB 15 degrees - 1cm ASA
IVC long axis
IVC short axis
Right anterior upper lung zone
Right anterior lower lung zone
Right PLAPs
Left anterior (upper and lower) lung zone
Left posterolateral lung zone
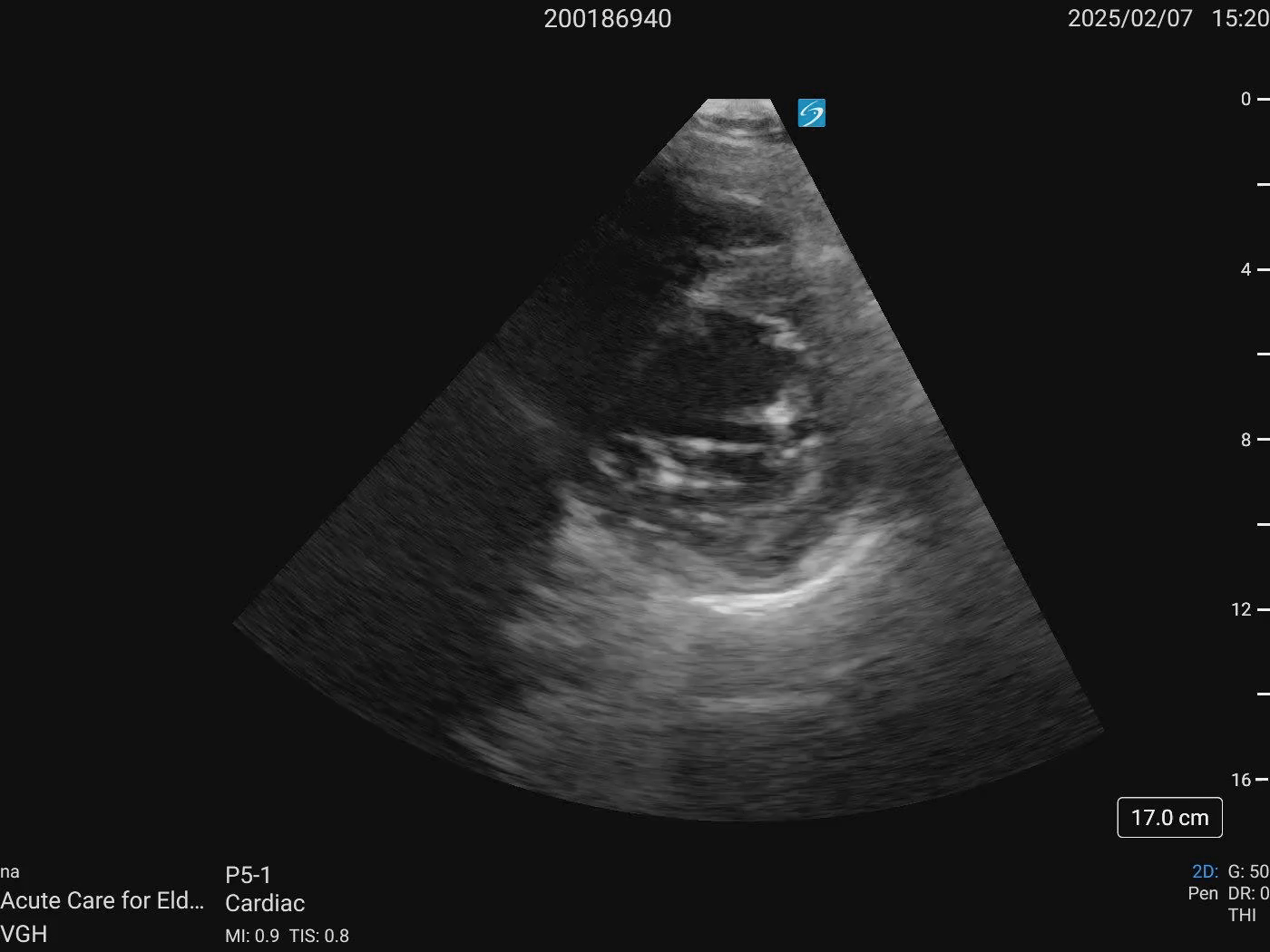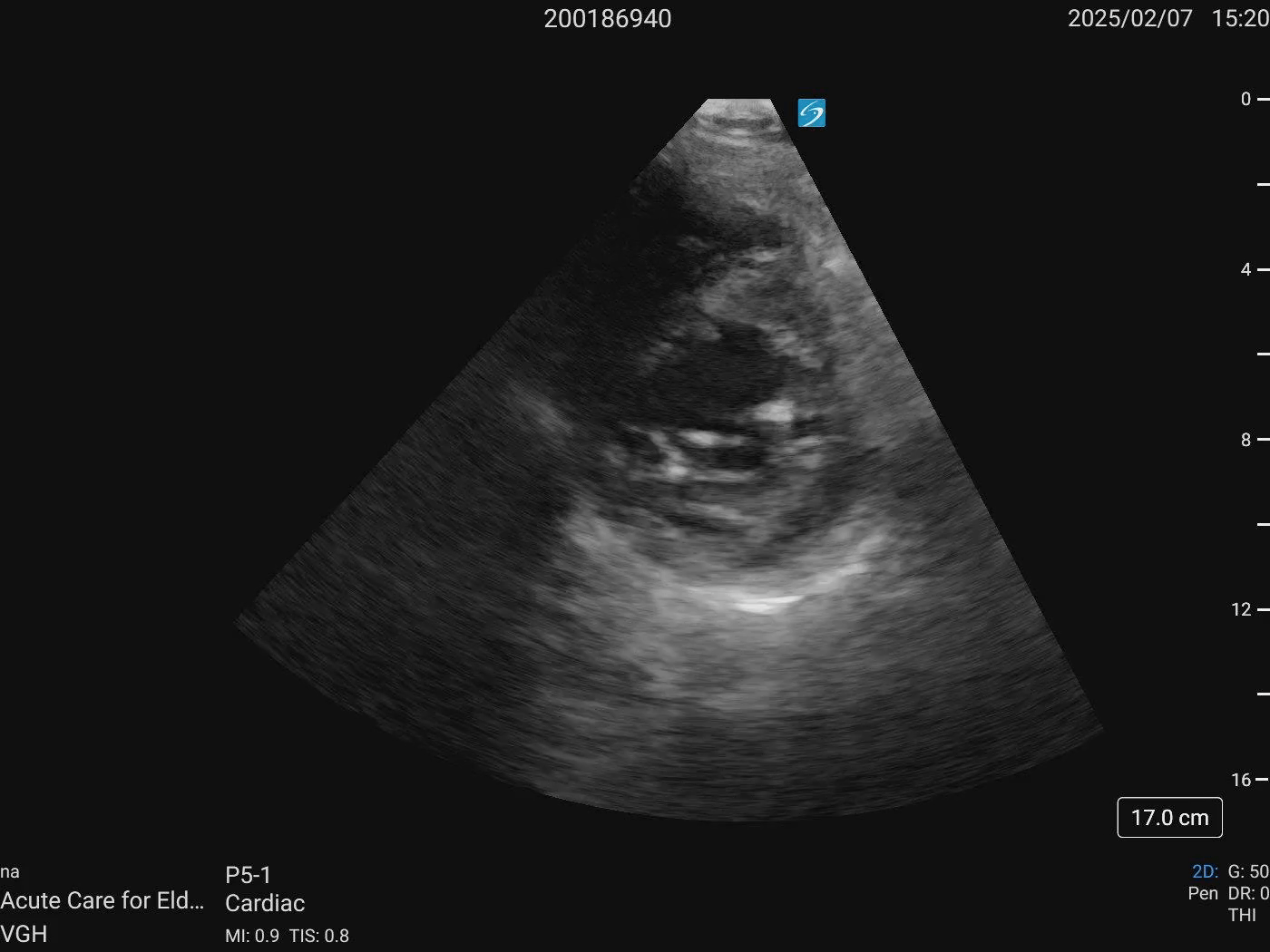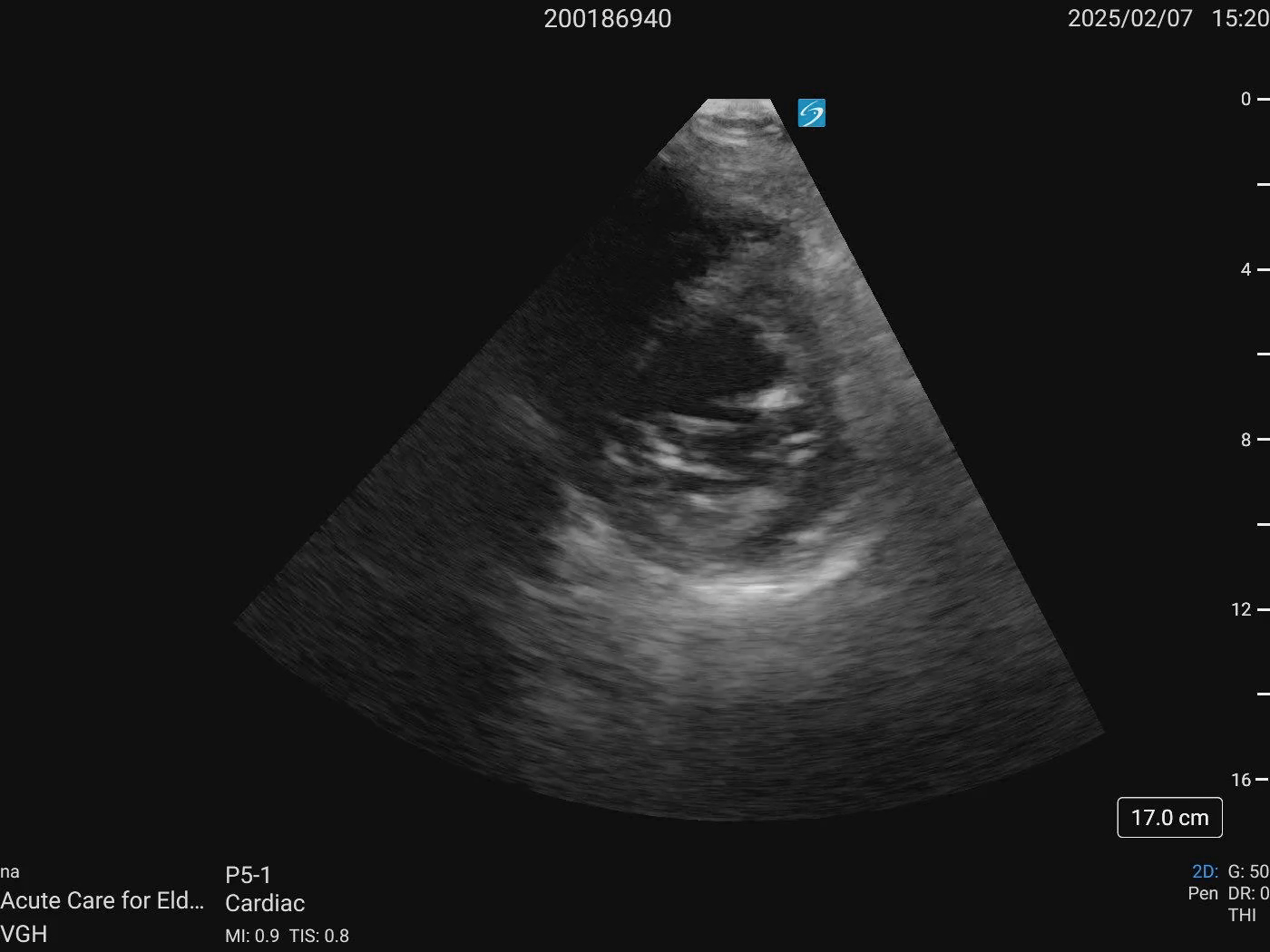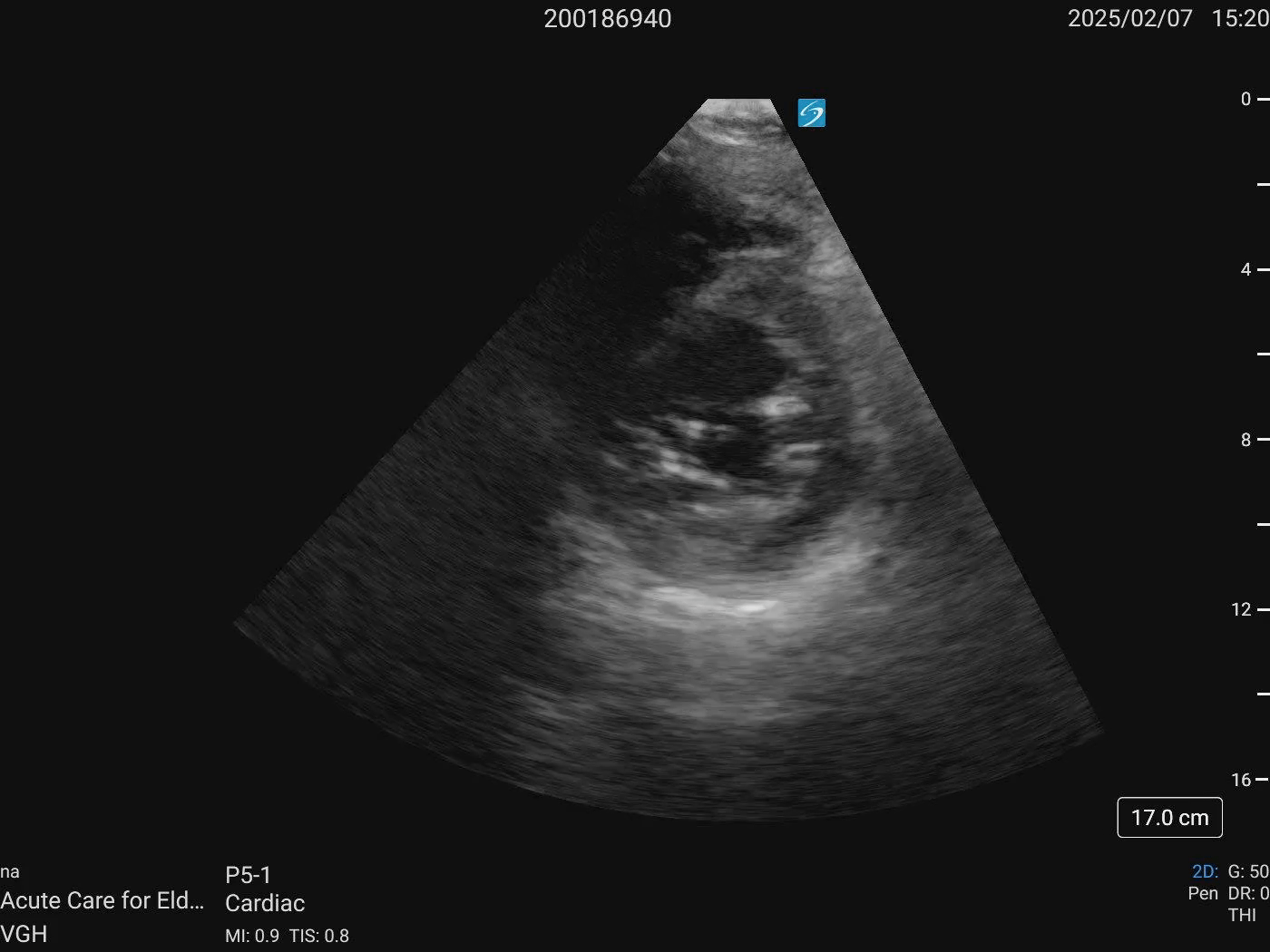
Cardiac ultrasound
PLAX
A5C
PSAX
VTI as high as 28
Mitral Valve Doppler
SUMMARY OF LUNG FINDINGS: Vertical artifacts
Distribution
Bilateral and multifocal
Patchy with skip areas
Greater density in the anterior lung zones (not a dependent gradient)
Characteristics of vertical artifacts
Predominantly broad and hazy of various widths and without discrete forms
Pleural line characteristics (associated with vertical artifacts)
Predominantly ragged / fragmented in appearance
Occasional subpleural consolidations
Regions of reduced pleural sliding
INTERPRETATION
Lung
Several characteristics associated with a non-cardiogenic interstitial process
Cannot r/o superimposed cardiogenic edema, however the lack of dependent vertical artifacts, pleural effusions and skip areas argue against a cardiogenic process
Substrate for discordant heart failure (elevated L sided filling pressures without elevated R sided filling pressures)
Normal RV function and size – RV tolerating LV dysfunction
Elevated L sided filling pressures in context of acute ischemic injury and AS and increase in PASP
Substrate for flash pulmonary edema
H/o acute ischemia, AS and acute LV injury impair L sided capacity to accommodate sudden changes in L sided volume and afterload
CO is likely sufficient with VTI measured here. SOB and kidney injury unlikely a forward flow problem
SUGGESTIONS
Agree with antibiotics for possible pneumonia
Suggest CT chest to help better characterize pattern of abnormalities and refine differential (non-cardiogenic interstitial process)
Pulmonary edema unlikely the primary driving factor for persistent resp symptoms, although it has likely played a role along the way
Patient remains total body overloaded and has demonstrated vulnerable to suspected sudden worsening of pulmonary congestion so ongoing diuresis as tolerated
However, given the fact that CVP is not elevated and Cr going up after > 1 week of high dose diuretics, this may be an indication that the vascular refill rate may be a limiting factor
CT Chest 6 days after consult
REspirology consult
Resp was consulted to review the CT chest findings that raised concern about organizing pneumonia
They felt resp symptoms likely multifactorial
Expanded infectious work-up
Given the fact that, if anything, his resp status was relatively stable there was any rush to initiating steroids
Suggested that pulmonary edema likely played a substantial role along the way
Case Continued
The patient had persistent respiratory symptoms (SOB, cough, sputum) with fluctuating O2 needs. He underwent cardiac catheterization which revealed severe prox-mid LAD disease and severe LCx disease. He was referred to CVSx but declined for surgery.
He ended up back in CCU for inotropic support to facilitate ongoing diuresis. He was placed back on HD for “brittle volume status and uremia”. Pip-tazo was restarted and a CT chest was repeated.
Repeat CT chest
Case Conclusion
Cardiology reviewed and in their latest note reported: “removed over 9L in CCU, still SOB, CHF less likely a driving cause”.
Respirology note: “it remains entirely possible that he does have organizing pneumonia - suggest initiating prednisone 60mg daily” (had been on 5mg daily after transplant)
Transplant ID suggested stopping pip-tazo: “has been on it a long time and doesn’t seem to be making a difference”
From notes 24-48hrs after starting prednisone: “Treated organizing pneumonia with prednisone. Much better today.”
DISCUSSION
There are many case reports of transplant-associated OP. For example:
4 Steps for Evaluating Vertical Artifacts
1.Distribution and density
Bilateral vs unilateral
Diffuse vs patchy (homogenous vs heterogenous)
Gravitational dependent pattern vs other
Number of vertical artifacts per ICS -> coalescing/lung white out
2.Vertical artifact characteristics (morphology)
Discrete vs broad and ill defined
Uniform brightness and extension vs variable in form
3.Pleural line characteristics (morphology)
Bright with thin, smooth contour vs ragged/interrupted with subpleural consolidations
Normal lung sliding vs reduced or absent lung sliding
4. Clinical integration
Cardiogenic vs non-cardiogenic
Difficult to r/o dual pathology (eg. ILD with superimposed pulmonary edema)
J Ultrasound Med 2023; 42:279-292